Vitamin D: Benefits, Deficiency, Foods, Toxicity, Side Effects & More
Vitamin D is a fat-soluble vitamin that has received increasing attention because of its proposed wide range of beneficial effects on the human body. Vitamin D is different from all the other nutrients in that the body can synthesize it in significant quantities with the help of sunlight. Therefore, vitamin D is not an essential nutrient. Given enough sun, people need no vitamin D from foods. This is why vitamin D is commonly referred to as the sunshine vitamin.

What is Vitamin D?
Vitamin D is a generic term for a family of compounds known as vitamins D1 (calciferol), D2(ergocalciferol) and D3(ergocalciferol). Chemically, these substances are called sterols, and their metabolic products have the ability to prevent rickets in children or osteomalacia in adults. Vitamin D is a fat-soluble steroid vitamin which functions to stimulate calcium uptake from the gut and its deposition in bone.
It is different from all other nutrients in that the body can synthesize it, with the help of sunlight, from a precursor that the body makes from cholesterol. Vitamin D comes in many forms, but only two of them are found in foods. They are:
Vitamin D2: vitamin D derived from plants in the diet. These can be found in certain types of mushrooms.
Vitamin D3: vitamin D derived from animals in the diet or made in the skin. These are mainly sourced from animal foods such as fat-laden fish and egg yolks.
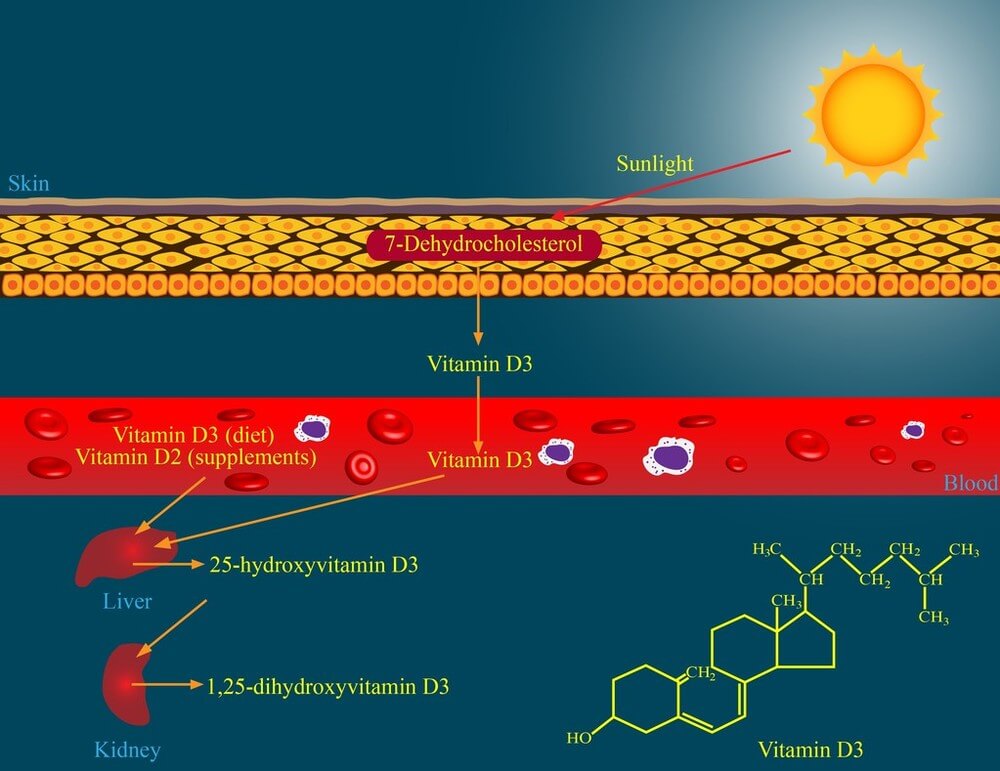
Vitamin D3 is the one that we should be really concerned with because it is twice as effective as Vitamin D2 in increasing the overall amount of Vitamin D in the blood. When ultraviolet rays shine on your skin, a cholesterol-like compound is converted into a precursor of vitamin D and absorbed into the blood. Over the next one and a half to three days, the precursor is converted to vitamin D3, an inactive form that is also called cholecalciferol. Vitamin D3 is converted into its active form by enzymes in the liver and then the kidneys.
The active form of vitamin D travels through the bloodstream to increase calcium (and also phosphorus) absorption in the intestine, decreases the amount of calcium excreted by the kidneys, and pulls calcium out of the bones when necessary. Blood calcium levels must be kept high so that enough calcium is present to build bones and teeth, contract and relax muscles, and transmit nerve impulses. Vitamin D works with other nutrients (such as vitamin A and C) and hormones to make and maintain bone.
As a fat-soluble vitamin, we do not need to ingest it every day, as it is stored in our liver. Vitamin D is the most toxic of all the vitamins but also the most stable. It is synthesised naturally from sunlight and your body will stop making vitamin D when you have enough stored. Calcium and phosphorus are needed for the utilisation of vitamin D, and vitamins A, C and E, protect vitamin D.
Health Benefits of Vitamin D
Vitamin D is currently one of the most widely researched vitamins, and this can be attributed to its proposed wide range of beneficial effects on the human body. Vitamin D has a major role in regulating the concentration of calcium and phosphate and promoting the healthy growth and remodeling of bone. It also has other effects, including some on cell growth, neuromuscular and immune functions, and inflammation.
Bone Health
Vitamin D is extremely important for enabling the absorption of calcium in your body. Considered a hormone, vitamin D is responsible chiefly for regulating the absorption and use of calcium and phosphorous and facilitating the formation of normal bones, cartilage, and teeth. Vitamin D regulates the supply of calcium in the blood and plays a role in the utilization of magnesium.
Vitamin D raises blood concentrations of bone minerals in three ways. When the diet is sufficient, vitamin D enhances their absorption from the GI tract. When the diet is insufficient, vitamin D provides the needed minerals from other sources: reabsorption by the kidneys and mobilization of the bones into the blood. The vitamin may work alone, as it does in the GI tract, or in combination with parathyroid hormone, as it does in the bones and kidneys.
Prevent Diabetes
Some research has found that vitamin D supplementation significantly reduces the risk of type 2 diabetes mellitus for non-obese pre-diabetic patients. Children treated with vitamin D have a lower incidence of type 1 diabetes. Conversely, vitamin D deficient children have an increased risk of developing type 1 diabetes. Vitamin D may also help prevent type 2 diabetes. Multiple studies have shown an inverse relationship between vitamin D levels and the incidence of type 2 diabetes. This may be due to a direct effect of vitamin D on insulin action, or it may be due to its effects on inflammation.
Protect the Heart
There also appears to be an increased risk of cardiovascular disease in patients with low vitamin D levels. A study found that individuals with low vitamin D levels had a 60% greater risk of cardiac events such as heart attacks and strokes, and when both a vitamin D deficiency and high blood pressure were present, the risk of a serious cardiovascular event was doubled. Increased vitamin D blood levels have been shown to decrease the risk of cardiovascular disease.
Boost the Immune System
Vitamin D functions to activate the innate and dampen the adaptive immune systems with antibacterial, antiviral, and anti-inflammatory effects. Vitamin D works as a hormone to regulate calcium metabolism. It also has an autocrine function, through which it facilitates gene expression in many cells. It is by the autocrine pathway, attached to the vitamin D receptor in cells, that vitamin D causes many effects, including modulation of immune function and neuromuscular function and reduction of inflammation. Vitamin D may also work via activated T and B lymphocytes, which are very important in the immune system.
Preventing Osteoporosis
Vitamin D and calcium should also be taken to prevent osteoporosis in patients at risk. Vitamin D is extremely important for enabling the absorption of calcium in your body. In the absence of calcium, your bones will weaken and become softer. This could lead to conditions such as osteoporosis. In addition to strengthening bones, vitamin D has also been shown to prevent falls, which may contribute to the decrease in fractures.
Reduces Cancer Risk
Some researchers theorize that vitamin D might aid in the prevention or treatment of cancer and assist in regulating the immune system. The vitamin D hormone is also capable of ensuring normal development of some cells, such as skin, colon, prostate, ovarian, and breast cells, in turn reducing cancer risk in these sites. Multiple epidemiologic studies have shown a higher rate of colon and breast cancer at higher latitudes, where vitamin D levels are lower.
Infection
At least one group of investigators has suggested that the reason for the increase in influenza (flu) during the winter is vitamin D deficiency from decreased sun exposure. Low vitamin D levels may contribute to reduced resistance to many types of infection, including tuberculosis.
Asthma
There is an association between lower maternal intake of vitamin D during pregnancy and the wheezing of children at ages 3 and 5. This may result in more children with asthma. Vitamin D is an essential nutrient with significant immunomodulatory effects. One review found that vitamin D supplementation could reduce the need for steroids used to inhibit episode frequency in people with mild to moderate asthma, and that supplementation had no effect on day-to-day asthma symptoms.
Alzheimer & Parkinson
Some observational studies have shown that lower serum vitamin D concentration is seen in most types of neurodegenerative disease, including Alzheimer’s disease, multiple sclerosis, and Parkinson’s disease. Vitamin D is a regulator of signal transduction and gene expression. It regulates calcium-sensing receptor expression, increases the clearance of β-amyloid peptides, and modulates inflammatory cytokine expression. Overall, vitamin D may play a beneficial role in Alzheimer’s disease. The metabolically active form of vitamin D3(calcitriol) is the most effective supplementation form of vitamin D in treating Alzheimer’s disease. In another study, it was shown that elevated mood and better cognition and memory in multiple sclerosis patients were associated with higher serum levels of vitamin D3.
Recommended Intakes for Vitamin D
International Units
Vitamin D was previously measured in international units, and so most nutrient composition tables use IU. The current AI for vitamin D is expressed in micrograms of cholecalciferol. The relationship between IU and micrograms of cholecalciferol is as follows:
1 IU = 0.025 microgram cholecalciferol
1 μg of cholecalciferol = 40 IU
The dietary reference intake for vitamin D issued in 2010 by the National Academy of Medicine, superseded previous recommendations which were expressed in terms of adequate intake. The recommendations were formed assuming the individual has no skin synthesis of vitamin D because of inadequate sun exposure. The tolerable upper intake level (UL) is defined as "the highest average daily intake of a nutrient that is likely to pose no risk of adverse health effects for nearly all people in the general population." Although ULs are believed to be safe, information on the long-term effects is incomplete, and these levels of intake are not recommended for long-term consumption.
| Vitamin D RDA in the United States | ||
| Age group | RDA (IU/day) | (μg/day) |
|---|---|---|
| Infants 0–6 months | 400* | 10 |
| Infants 6–12 months | 400* | 10 |
| 1–70 years | 600 | 15 |
| 71+ years | 800 | 20 |
| Pregnant/Lactating | 600 | 15 |
| Age group | Tolerable upper intake level (IU/day) | (μg/day) |
| Infants 0–6 months | 1,000 | 25 |
| Infants 6–12 months | 1,500 | 37.5 |
| 1–3 years | 2,500 | 62.5 |
| 4–8 years | 3,000 | 75 |
| 9+ years | 4,000 | 100 |
| Pregnant/lactating | 4,000 | 100 |
Upper Level for Vitamin D
The upper level for vitamin D is 100 micrograms per day (4000 IU per day). This is the perfect amount for people who are suffering from Vitamin D deficiency. It is not uncommon for doctors to recommend a higher dosage than that. Too much vitamin D taken regularly can create problems, especially in some infants and young children. For adults, intakes somewhat above the upper level appear to be safe. The upper level is based on the risk of too much vitamin D causing the overabsorption of calcium, which eventually leads to calcium deposits in the kidneys and other organs. These high intakes of vitamin D would also cause the typical symptoms of high blood calcium: weakness, loss of appetite, diarrhea, vomiting, mental confusion, and increased urine output. Calcium deposits in organs cause metabolic disturbances and cell death.

Symptoms Of Vitamin D Deficiency
Vitamin D deficiency or hypovitaminosis D is a vitamin D level that is below normal. It most commonly occurs in people when they lack sufficient exposure to the sun or have an inadequate nutritional intake of vitamin D. Vitamin D deficiency causes hypocalcemia and hypophosphatemia, or diminished blood levels of calcium and phosphorus. The deficiency in turn causes stimulation of the parathyroid gland. The hormone secreted by the gland pulls calcium out of bones to restore the calcium in the blood to adequate levels. This process causes rickets in infants and children, and osteomalacia in adults.
Osteomalacia and Rickets
Rickets is a disease of toddlers whose bones are undermineralized as a result of poor absorption of calcium in the absence of adequate amounts of calcitriol. When the child begins to walk, the long bones of the legs are deformed, leading to bow-legs or knock knees. More seriously, rickets can also lead to collapse of the ribcage and deformities of the bones of the pelvis. Similar problems may also occur in adolescents who are deficient in vitamin D during the adolescent growth spurt, when there is again a high demand for calcium for new bone formation.
Osteomalacia is the adult equivalent of rickets. It results from the demineralization of bone, rather than the failure to mineralize it in the first place, as is the case with rickets. Women who have little exposure to sunlight are especially at risk of developing osteomalacia after several pregnancies because of the strain that pregnancy places on their marginal reserve of calcium.
Osteomalacia also occurs in older people. Here again, the problem may be inadequate exposure to sunlight, but there is also evidence that the capacity to form 7-dehydrocholesterol in the skin decreases with advancing age, so that older people are more reliant on the few dietary sources of vitamin D.
Although vitamin D is essential for the prevention and treatment of osteomalacia in older people, there is less evidence that it is beneficial in treating the other common degenerative bone disease of advancing age, osteoporosis, which is due to a loss of bone matrix rather than an enhanced release of calcium from bone with no effect on the organic matrix, as is seen in osteomalacia. The result is negative calcium balance and loss of bone mineral, but secondary to the loss of organic matrix, owing to the progressive loss of estrogens and androgens, rather than a failure of the vitamin D system.
In most cases, vitamin D deficiency is almost asymptomatic. It may only be detected on blood tests but is the cause of some bone diseases and is associated with other conditions:
- Hypocalcemia: muscle aches, weakness, and twitching
- Bone pain
- Periodontitis
- Increased risk of fracture
- Respiratory infections
- Schizophrenia
Populations at risk for vitamin D deficiency
- Infants: Infants constitute a population at risk for vitamin D deficiency because of their relatively large vitamin D needs brought about by their high rate of skeletal growth.
- Adolescents: A period of rapid growth of the skeleton occurs at puberty. Insufficient vitamin D stores during this period of increased growth can lead to vitamin D insufficiency.
- Elderly: Elderly people have a higher risk of having a vitamin D deficiency due to a combination of several risk factors, including decreased sunlight exposure, decreased intake of vitamin D in the diet, and decreased skin thickness, which leads to further decreased absorption of vitamin D from sunlight.
- Obesity: Vitamin D is stored in fat, and with large amounts of fat, large amounts of the vitamin can be in the fat and not available to the body for use.
- People with dark skin: Groups with darker skin because of increased pigmentation make less vitamin D in the skin. Vitamin D deficiency is seen more frequently in ethnic groups with darker skin.
- People with trouble absorbing fat, since vitamin D is a fat-soluble vitamin. This could include people with cystic fibrosis as well as Crohn’s disease. After gastric bypass surgery, vitamin D absorption is reduced.
- Residents at higher latitudes, where there may not be enough sun exposure during part of the year to make vitamin D.
Vitamin D Toxicity & Side Effects
Since vitamin D is fat soluble, too much vitamin D can be toxic because it can build up and affect the soft tissues of the body. An overdose usually comes from dietary supplements, not food—and not from overexposure to sunlight. The amounts of vitamin D made by the skin and found in foods are well within safe limits, but supplements containing the vitamin in concentrated form should be kept out of the reach of children. Young children and infants are especially susceptible to the toxic effects of too much vitamin D.
Vitamin D in excess is the most toxic of all the vitamins. It enhances calcium absorption, produces high blood calcium, and promotes the return of bone calcium into the blood and the release of calcium from the skeleton. The excess calcium then tends to precipitate in the soft tissues, forming stones, including kidney stones. Calcification may also harden the blood vessels and is especially dangerous in the major arteries of the brain, heart, and lungs, where it can cause death. A vitamin D overdose can cause the following symptoms:
- Hypercalcemia (Anorexia, Nausea, and Vomiting)
- Polyuria (Excess Urination)
- Polydipsia and Thirst
- Weakness, Insomnia
- Hyperparathyroidism
- Kidney Disease
- Artherosclerosis
- Intellectual Disability in Young Children
- Abnormal Bone Growth
- Severe Depression

Best Source of Vitamin D
Vitamin D from the Sun
Most of the world’s population relies on natural exposure to sunlight to maintain adequate vitamin D nutrition. The body can make vitamin D after sunlight, or ultraviolet light, hits the skin, even on cloudy days. The sun imposes no risk of vitamin D toxicity.
For most people, exposing their hands, faces, arms, and legs on a clear summer day for 10 to 15 minutes, twice weekly, should be sufficient to maintain vitamin D nutrition. Dark-skinned people require longer exposure than light-skinned people.
Caution: Prolonged exposure to sunlight has other undesirable consequences, however, such as premature wrinkling of the skin and skin cancers. Routinely protect your skin after those 10 to 15 minutes with sunscreen that has an SPF of 15 or more!
For older adults, people with dark skin, and people exposed to insufficient ultraviolet light, additional vitamin D intake from vitamin D fortified foods or supplements is recommended.
Food Sources of Vitamin D
- Rich sources are fatty fish: sardines, salmon, herring, trout, tuna, eel, mackerel, Atlanta herring, Fish Liver oils
- Butter
- Fortified milk: milk is also an important source of dietary calcium
- Eggs: egg yolks
- Liver: the liver and fat from mammals living in and around cold water
- Mushrooms
- Some cereals
Drug Interactions
The cholesterol-lowering drug cholysteramine and mineral oil both interfere with the intestinal absorption of vitamin D. Phenytoin and phenobarbital, drugs used in the treatment of seizures, speed up the metabolism of vitamin D.
Most problems with the use of vitamin D interacting with other drugs occur in the presence of hypercalcemia (elevated blood calcium levels) and heart or kidney disease. Heart irregularities may occur with the use of digoxin and other digitalis derivatives or verapamil. In the presence of elevated calcium levels associated with the vitamin’s use, arrhythmias (heart irregularities) may occur. Thiazide diuretics in the presence of vitamin D may cause hypercalcemia in the presence of hypoparathyroid disease. People with kidney failure should avoid taking magnesium-containing antacids with vitamin D.